The incidence of pancreatic cancer is increasing worldwide and currently almost half a million people are diagnosed with this disease each year. For most patients with a pancreatic cancer, the tumor is located in the pancreatic head. The complex ‘Whipple’ (i.e. pancreatoduodenectomy) procedure is the most common surgical procedure performed to remove this cancer in the head of the pancreas and improve the life expectancy of patients.
During Whipple surgery, a localized tumor is removed to restore the flow of pancreatic digestive fluids and bile from the liver into the digestive tract. It is a complex surgery in which the head of the pancreas, the first region of the small intestine (i.e. duodenum), and the gallbladder with the distal bile duct are removed, while preserving major blood vessels in the area. Importantly, the three-way junction between the remaining organs needs to be restored carefully to support normal digestion and prevent complications such as leakage of digestive fluids into the abdominal cavity.
Over recent years, significant progress has been made to improve the quality and safety of the Whipple procedure, thanks to formidable efforts by collaborative surgical clinical research. A considerable contribution to this research was initiated in the Netherlands by the Dutch Pancreatic Cancer Group (DPCG). The DPCG is a national multidisciplinary collaboration that brings various experts together, including surgeons, oncologists, radiologists, pathologists, and scientists. The hepato, pancreatic, and biliary (HPB) surgical team at Cancer Center Amsterdam – Amsterdam UMC is also part of the DPCG.
How Are New Surgical Techniques Implemented?
Long gone are the days when new surgical techniques were introduced in an operating theater on a whim, after watching a surgical video or even a one-day course. “Compare it to traveling by plane,” Marc Besselink, Professor of Pancreatic and Hepatobiliary Surgery, starts off. “When you board, you expect the pilots, crew, and ground staff to be properly trained and certified. The same holds true for what patients can expect from surgeons and the teams running the operating room. The patient is trusting you with their life. Obviously, the facilities and staff should be highly trained, experienced, and top notch.”
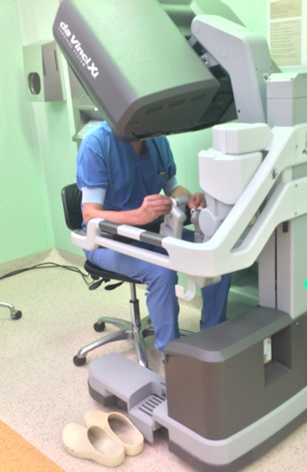
Training Programs and Randomized Trials to Improve Minimally Invasive Pancreatic Surgery
- (2016) Impact of a Nationwide Training Program in Minimally Invasive Distal Pancreatectomy
- (2019) Minimally Invasive Versus Open Distal Pancreatectomy: A Multicenter Patient-blinded Randomized Controlled Trial
- (2019) Minimally Invasive versus Open Distal Pancreatectomy for Ductal Adenocarcinoma: A Pan-European Propensity Score Matched Study
- (2019) Outcomes of a Multicenter Training Program in Laparoscopic Pancreatoduodenectomy
- (2019) Laparoscopic versus open pancreatoduodenectomy for pancreatic or periampullary tumours: a multicentre, patient-blinded, randomised controlled phase 2/3 trial
- (2022) Outcomes of a Multicenter Training Program in Robotic Pancreatoduodenectomy
Beyond the ‘one-size-fits-all’ approach
“We are passionate about our mission to keep pushing boundaries to improve patient care. This starts with careful and objective evaluation of techniques and outcomes to see how the surgery can be improved. We also look at treatment modality. For example, can pretreatment with chemotherapy allow more patients to be helped by the Whipple procedure? How can we tailor this particular surgery to the needs of each patient?” says Prof. Besselink.
Volume Matters
Several studies from research groups in the United States clearly highlighted that minimally invasive Whipple surgery only improves outcomes when performed at least 20 times per medical center per year. If performed less, outcomes were generally worse compared to the traditional, open surgical approach.
Prof. Besselink: “This finding really opened our eyes and led directly to new guidelines. The Miami guidelines, in which the Dutch team was closely involved, now states that minimally invasive Whipple surgery should be limited to hospitals that perform at least a total of 50 Whipples procedures (open and/or minimally invasive) each year.” This advice excludes roughly 80% of the hospitals in Europe and has accelerated centralization of these complex surgeries in select expertise centers, including Amsterdam UMC.
This guideline is essential for good clinical practice, according to Prof. Besselink: In Germany – without centralization of complex care – the surgery-associated mortality following the days and weeks after a Whipple procedure exceeds 10%. In the United States, over 80% of surgeons performing Whipple surgery perform less than two of these operations per year, resulting in unacceptable outcomes.
In the Netherlands, the current minimum volume requirement for Whipple surgery is 20 procedures per center per year. Since the implementation of the new guidelines, the mortality following Whipple surgery has dropped to 3 percent. This result is also supported by recent nationwide research of the Dutch Pancreatic Cancer Group. At Amsterdam UMC, following the merger between AMC and VUmc hospitals, over 140 of these procedures are now performed annually, leading to enhanced care pathways and highly specialized teams resulting in a further reduction in mortality.
Robot-assisted Whipple: The Pittsburgh Connection
Eight of the 16 hospitals performing pancreatic surgery in the Netherlands also met the new guideline-based volume requirement for participation in LEALAPS-3. The objective of this study was to assess feasibility and safety of a multicenter training program in robot-assisted pancreatoduodenectomy based on techniques developed by surgeons in Pittsburgh, Pennsylvania.

From left to right: Prof.Marc Besselink - Shirley Sussenbach - Maurice Zwart - Dr. Melissa Hogg (Pittsburgh, currently Chicago), and Prof. Olivier Busch.
The intensive training program involved 100 hours of surgical videos followed by training on a robotic virtual simulator, in which participating surgeons had to achieve a quality score of 95% in 20 robot-assisted surgical exercises. This was followed by comprehensive simulation exercises with plastic-silicone mockups to practice suturing. Only then were trainees allowed to operate under supervision on patients using the surgical robotic system.
Prof. Besselink: “Three Pittsburgh-based surgeons came to the Netherlands to instruct us.Following that, our PhD student tra velled with them to all participating pancreatic centers in the Netherlands to train surgeons there. Thanks to the Pittsburgh training program, we had a very quick - and most importantly - safe dissemination of knowledge and skills that resulted in multiple medical centers gaining solid expertise in robot-assisted Whipple surgeries. Currently the use of robotic Whipple surgery in the Netherlands is the highest in the world, exceeding 25%.”
To further evaluate the new procedure, a randomized controlled trial called ‘DIPLOMA-2’ is ongoing that includes 288 patients, two-third of these patients are randomly selected for robot-assisted Whipple surgery versus one-third for standard open Whipple. “The study aims to confirm the safety of this approach and objectify potential benefits. Thirteen centers in the Netherlands, Italy, Belgium, Germany, and Sweden are participating, and the trial is well ahead of schedule. At this time, over 90% of patients have been included over 17 months, and results are expected by the end of this year:” says Prof. Besselink.
Passing it on! EU-wide Training Program
Following the successful introduction of the robot-assisted Whipple procedure at Cancer Center Amsterdam and select hospitals in the Netherlands, countries across Europe started to take notice. “It was time to pass on the expertise we had gained,” says Marc. Thus, the European LEARNBOT program was launched.
This training program is endorsed by the European-African Hepato-Pancreato-Biliary Association (E-AHPBA), a ‘prime interdisciplinary organization for HPB-related surgical science and scholarship in the Europe-Africa-Middle-East region’ (see below ‘Prof. Marc Besselink Appointed President’). Eligible hospitals were invited to join the training program free of charge. The only requirement is that surgical parameters are submitted to the European surgical ‘E-MIPS’ quality audit to monitor quality and give feedback.
Inspiring International Experiences in the Operation Theater
“The LEARNBOT experiences are truly enthralling and a wonderful boost for all the members of our operation room team at Amsterdam UMC and other centers involved,” Prof. Besselink says enthusiastically. “For instance, every Monday here at Cancer Center Amsterdam, we start a robotic Whipple surgery procedure with two operating pancreatic surgeons. Next to myself Prof.Olivier Busch, Dr.Sebastiaan Festen (OLVG, HPB-Amsterdam collaboration), and Dr.Freek Daams." For the majority of procedures, this involves a training session with a different international team of surgeons sometimes accompanied by their ‘scrub’ nurses. Already, 50 teams from leading medical centers such as Milan, Stockholm, Heidelberg, Paris, Berlin, and Copenhagen - have visited us.”
Each Monday, the operation room is filled with anticipation, who will visit this week? “We have welcomed surgeons from across Europe, including Finland, the Czech Republic, Poland, but also China, Malaysia, and the United States. And in many of these occasions, we actually learn from each other with new surgical concepts and ‘technical tricks’ being discussed afterwards over a cup of soup. It is very inspiring to us all, knowing that patients with pancreatic cancer all over Europe, and even further away, can rely on their surgeons following dedicated training programs and sharing experiences and knowledge. As an operation room team, it inspires us greatly. Our guests show great appreciation for the good atmosphere, smooth teamwork team, and communication between anesthetists, ‘scrub’ nurses and surgeons.”

Next Steps in Robot-Assisted Surgery
At Amsterdam UMC, work is ongoing to add a fourth robot to the three existing Da Vinci Intuitive robots. The expansion will support further implementation of robot-assisted operations in other disciplines like pulmonary, colorectal, gynecological, esophageal, and gastric surgery. Recently, new robotic systems from different manufacturers have become available which allows for comparison of important aspects like costs and sustainability.
In the meantime, PhD students at Cancer Center Amsterdam, who also work in Brescia, Italy, for the “European Consortium on Minimally Invasive Pancreatic Surgery” (E-MIPS) are analyzing data from over 4000 surgeries included in the E-MIPS European quality registry. Prof. Besselink: “Just because you become an expert in the latest state-of-the-art technique doesn’t mean you are done. You have to continue to push those boundaries. That is why we require teams we train to submit all data to the audit for quality monitoring. It is vital to complete the quality cycle to spot whether clinical practice is in agreement with clinical trial results, and to evaluate where the next improvements can be made that will help our patients.”
Prof. Marc Besselink Appointed President of the E-AHPBA
After being president-elect for two years, Prof. Marc Besselink will be appointed president of the European-African Hepato-Pancreato-Biliary Association (E-AHPBA) on June 8, 2023. The idea to bring HPB surgeons for Africa, Europe, and the Middle East together in the E-AHPBA originated in 1990. Currently, E-AHPBA has over 1000 active members representing national HPB organizations from the Czech Republic, Egypt, France, Germany, Great Britain and Ireland, Greece, Italy, Kenya, MENA (Middle East and North Africa), the Netherlands, Scandinavia, Spain, South Africa, Turkey, and Russia.
Prof. Besselink will be the youngest president to serve E-AHPBA and will act in this role for two years to preside over key executive and council responsibilities, supervise the management bureau and interactions with sponsors, and will be closely involved in the organization of the annual congress. He will also coordinate interactions and data sharing with the Americas Hepato-Pancreato-Biliary Association (AHPBA) and the world organization IHPBA.
In his mission as E-AHPBA president, Prof. Besselink will focus on:
- The program aims to train and mentor younger surgeons in affiliated countries.
- This involves the implementation of an exchange program supporting professionals from both sides of the Atlantic to visiting each other's locations, sharing expertise, and organizing joint events such as ‘a best-of-the-best showcase’ at respective congresses.
- E-AHPBA is emphasizing a more structured approach to training in robotic surgeries for both pancreas and liver. Amsterdam UMC plays a central role in these efforts.
Prof. Geert Kazemier, Chair of the Executive Board Cancer Center Amsterdam: “This appointment also highlights Amsterdam UMC’s central role in advancing the care of patients with pancreatic and liver cancer through Europe and beyond. Congratulations to Prof. Marc Besselink on being appointed president of the E-AHPBA.”
For more information, contact Prof. Marc Besselink.
People involved at Amsterdam UMC – Cancer Center Amsterdam
Prof. Olivier Busch, HPB surgery
Prof. Geert Kazemier, HPB surgery
Dr. Freek Daams, HPB surgery
Dr. Sebastiaan Festen, HPB Surgery (also: OLVG, HPB-Amsterdam)
Dr. Babs Zonderhuis, HPB surgery
Dr. Joris Erdmann, HPB surgery
Dr. Rutger-Jan Swijnenburg HPB surgery and proctor robotic liver surgery
Annuska Schoorlemmer, nurse specialist HPB surgery
Andre Sterk, nurse specialist HPB surgery
Dr. Rogier Voermans, gastroenterology HPB
Dr. Roy van Wanrooij, gastroenterology HPB
Dr. Thijs Wielenga, gastroenterology HPB
Dr. Maarten Jacobs, gastroenterology HPG
Prof. Paul Fockens, gastroenterology HPB
Irma Post-Hoekstra nurse specialist HPB gastroenterology
Prof. Hanneke Wilmink, medical oncology pancreas
Dr. Heinz-Josef Klumpen, medical oncology liver
Mariette Weterman, nurse specialist HPB oncology
Prof. Otto van Delden, interventional radiology HPB
Prof. Martijn Meijerink, interventional radiology HPB
Dr. Janneke van den Bergh, radiology HPB
Prof. Jaap Stoker, radiology HPB
Prof. Joanne Verheij, pathology HPB
Dr. Arantza Farina, pathology HPG
Fritz de Graaf, lead operating team robotic surgery HPB
Els Jagtenberg, lead operation planning
Marie-Jose Hendriks, lead patient ward 6B
Chris Bakker, lead patient ward 6C
Drs. Maurice Zwart, PhD Student LAELAPS-3
Dr. Jony van Hilst, post-doc LAELAPS, DIPLOMA
Drs. Leia Jones, PhD student LEARNBOT
Drs. Anouk Emmen, PhD student DIPLOMA-2
Drs. Nine de Graaf, PhD student DIPLOMA-2
Text by Henri van de Vrugt.
This article was created for Cancer Center Amsterdam.
© 2023 NHBC– All rights reserved.

