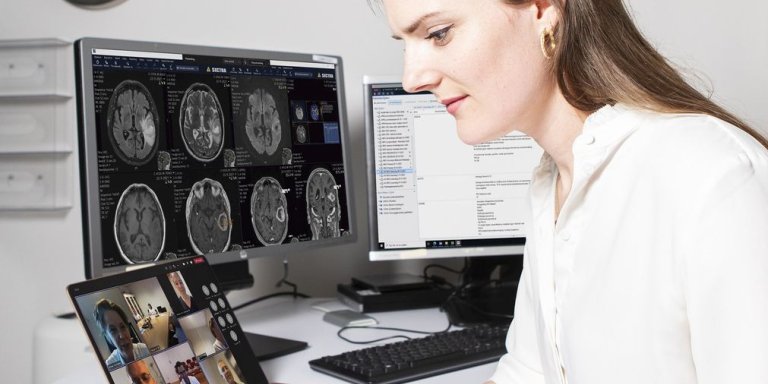
“The triage panel comprises all the specialists needed to arrive at a well-founded treatment recommendation: a neurologist, a neurosurgeon, a radiologist, and in the later stages a radiotherapist and a medical oncologist,” says Merijn de Swart, the physician-scientist who set up the triage panel. She is the first author of a scientific article on the project which was recently published in the journal Neuro-Oncology Practice.
How does the panel operate?
The panel uses a digital platform, to which the patient’s neurologist uploads the scans available, accompanied by a completed registration form containing all the relevant patient information. The patient’s case is discussed at a regional multidisciplinary meeting that takes place three times a week.
On the day of the meeting, the triage panel sends feedback to the referring physician, who discusses the recommendation with the patient. If they both agree, an outpatient clinic appointment or clinical transfer is scheduled. “This makes the diagnosis and the plan of attack clear for both the patient and the referring physician much faster than in the traditional referral system,” says De Swart.
The old situation
In the Netherlands, brain tumors are treated at specialist centers, one of which is Amsterdam UMC’s Brain Tumor Center. Referrals from regional hospitals were traditionally sent by email and fax, with the result that the information was scattered across various channels. “Often the letter does not arrive at the same time as the CD-ROM of the MRI scan. Tracking the two down is time-consuming, not to mention error-prone,” explains Maaike Schuur, a neurologist at the Brain Tumor Center who took part in the study.
An additional problem is that the patient’s clinical data in the referral note are often incomplete. As Schuur says, “That means we do not have sufficient information on the person’s general physical condition, which we need to come up with a good treatment recommendation. Can the patient be sent to a neurosurgeon immediately, or are there other problems – epilepsy, for instance – that require a neuro-oncologist to assess the case as well?”
Traditional obstacles to speed
When consultations between the attending neurologist and the neuro-oncologist or neurosurgeon at the Brain Tumor Center took place by phone – in urgent cases, for example – the Brain Tumor Center was unable to access the MRI scan from the regional hospital. Instead, the hospital sent a few images from the scan by email, or a courier delivered a CD-ROM of the scan to Amsterdam UMC.
Because of these obstacles, the traditional route – from the initial scans to a patient with a growth in the brain being received at the Brain Tumor Center – took six days. The time between the initial scan at the regional hospital and the start of any treatment was 27 days. “All that time, the patient is left in a state of great uncertainty, which is emotionally draining,’’ says Schuur.
Time-saving
Four regional hospitals (Dijklander, OLVG, Tergooi and Zaans Medical Center) were therefore interested in the project to speed up this referral process using a digital platform and a multidisciplinary triage panel.
“One result of having cases discussed by the triage panel was that far more patients were referred straight to a neurosurgeon, whereas with the traditional referral route they were seen by the neurologist first and only later by the neurosurgeon. That produced a time-saving.”
The referral time for the 72 patients assessed by the triage panel during the study was not six days, as with the traditional route, but only one day. The time between the initial scan and the start of treatment went down from 27 days to 15. “There was no difference between this approach and the normal referral route in terms of cost and time investment,” notes De Swart.
More hospitals joining the scheme
Neurologist Cathelijne Gorter de Vries of the Zaans Medical Center is enthusiastic about the new system. Nowadays it is standard practice for her to consult the triage panel when a primary brain tumor is suspected, and she no longer sends CD-ROMs by mail. “It’s great that, even in the initial uncertain phase at our hospital, we can broadly outline what the treatment process will be at Amsterdam UMC. That gives patients something to hold on to at an anxious time. We cannot remove the uncertainty entirely, however, as the nature of the tumor and the final treatment plan will only become clear after surgery and the neuropathology tests.”
Gorter de Vries is also pleased that she can do more for patients with whom she has a great deal of contact. “Some patients are admitted to the Zaans Medical Center for one or two weeks of tests, and I usually see them every day. That creates a bond. As long as they are with us, I want to support them as best I can. That’s easier now, thanks to the triage panel.”
Now that the study has finished, these satisfactory results mean that the neuro-oncology triage panel is being continued and implemented as part of regular care. Amsterdam’s BovenIJ Hospital and the Flevo Hospital in Almere have meanwhile joined the scheme that provides advice on referrals.
This is a translation of a condensed version of an article in JANUS, the popular scientific magazine of Amsterdam UMC
Photo of Merijn de Swart during a digital triage panel: Martijn Gijsbertsen