In medical terms, ‘triage’ means to quickly assess a medical condition to decide the urgency of treatment. Researchers at the Brain Tumor Center Amsterdam recently published the results of their quality improvement initiative in the journal Neuro-Oncology Practice. This study was the first-ever published initiative in the field of neuro-oncological care that improved the referral management with an online data sharing platform.
Standard referrals
The majority of patients with neurological symptoms first report to an emergency room or outpatient clinic at a general hospital. Patients with suspected neuro-oncological disease are then referred to the Brain Tumor Center Amsterdam, a process involving a cumbersome transfer of images on CD-ROM by mail or courier service.
To improve the referral management of brain tumor patients, neurologists Dr. Mathilde Kouwenhoven, Dr. Tjeerd Postma, Dr. Maaike Schuur and neurosurgeon Prof. Philip de Witt Hamer initiated an online data sharing platform and multidisciplinary triage panel including neurologists, neurosurgeons, radiologists, and, since the COVID-19 pandemic, radiation oncologists. “Timely referrals in cancer care are really important as delays may affect emotional distress, treatment outcome, and even survival,” says first author Merijn de Swart. “Brain tumor patients are vulnerable due to the possible rapid progression of symptoms.”
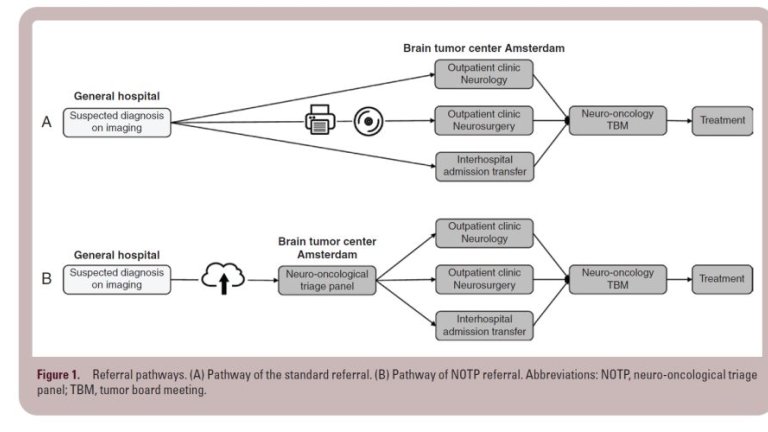
Image adapted from de Swart et al. (2021)
Streamlining referrals
Supported by the CitrienFund’s ‘Moving towards Regional Oncology Networks’ program, the neuro-oncological triage panel established these key points to streamline the referral pathway:
- A secure online data-sharing platform to share patient information and diagnostic imaging between participating centers in the region and Brain Tumor Center Amsterdam. In standard practices, the lack of electronic access to patient information and diagnostic imaging across healthcare organizations could hinder interhospital consultation and referral.
- A novel standardized registration form that included all essential information for the multidisciplinary triage panel to be able to discuss the patient and provide substantiated advice.
- Triage meetings were integrated into preexisting neuroradiology meetings. This minimized health care professionals’ time effort while tailoring the patient referral based on the collective advice from the triage panel.
Implementation in three phases
The neuro-oncological triage panel was implemented in three phases. In phase 1, three general hospitals in the Amsterdam area were connected to the secure online data-sharing platform (the EVOCS®-network). Neurologists from these centers could digitally refer patients to the neuro-oncological triage panel. After 6 months, the workflow and satisfaction of the participating centers were evaluated via site visits. This resulted in only minor tweaks to the registration form. In the second implementation phase, digital access to the neuro-oncological triage panel was expanded to two other general hospitals, followed by three additional hospitals in the third phase for a total of eight participating hospitals.
Reducing lead times without increasing costs
Between February 2019 and March 2020, 225 newly-diagnosed patients were referred to The Brain Tumor Center of Amsterdam UMC: 153 had a standard referral and 72 had a digital referral via neuro-oncological triage panel.
Patients discussed in the neuro-oncological triage panel were referred more frequently for a neurosurgical consultation. Time-to-referral was reduced from 6 days to 1, and total time-to-treatment was decreased from a median of 27 days for the standard referral group to 15 days for the digitally referred group. Costs and time investment were comparable for both groups.
What next?
This study shows that implementation of digital referral through a multidisciplinary neuro-oncological triage panel improved regional referral management. What is happening with the panel now? The triage panel has continued with minor modifications due to the pandemic, according to the authors of the study. They note that the pandemic may have given the initiative a bit of a boost as physical outpatient access to medical facilities was severely restricted and tele-consultation became essential.
Digital patient data sharing across health care facilities in the Netherlands has been rapidly developing, and digital image exchange between the majority of Dutch hospitals has been feasible for a couple of months. In the future, the ultimate goal is to achieve digital access to a triage panel regardless of the hospital of diagnosis. The neuro-oncological triage panel has provided a feasible and valuable blueprint that can be generalized to other oncological care pathways requiring the collaboration and coordination of multiple medical specialties.
For more information see the article or contact: m.deswart@amsterdamumc.nl