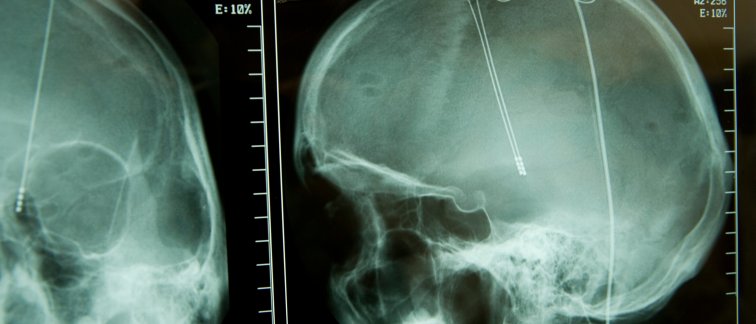
The minimally conscious state (MCS) is a prolonged disorder of consciousness (PDOC) after coma that can be caused by severe brain injury. MCS is the state in which a person shows clear but minimal and inconsistent awareness. Although MCS patients show noticeable intended behavior, and exhibit signs of minimal self-awareness and awareness of their environment, they are incapable of adequate and consistent responses to the outside world. Medical care for these patients is mainly supportive, as treatment options remain scarce.
Attempts to improve consciousness
Since the early 1960’s there have been several attempts to improve arousal and awareness in patients with prolonged disorder of consciousness using DBS. As the results from these studies vary from literally no effects of stimulation to rather spectacular improvements of consciousness, it remains unknown what the exact underlying DBS mechanisms are, causing its effects on human consciousness and why these effects are so widespread.
Low-frequency, high impact
In the study of Hisse Arnts, the clinical and neurophysiological effects of DBS were observed in a single patient with MCS, more than eight years after brain injury. The researchers performed an experimental trial for 24 months of DBS targeted at the central thalamus, with different stimulation settings, varying in pulse-width and two different stimulation frequencies (50 Hz and 130 Hz). Magnetoencephalography (MEG) was used to measure the DBS-induced changes in neuronal activity and functional interactions between brain regions.
DBS was associated with signs of increased arousal, visual pursuit (such as recognition of family members), return of swallowing, and reduction of spasticity. Watch the video in the published paper where DBS is activated and deactivated (scroll almost all the way down). Moreover, DBS was associated with an increase in functional connectivity and neural variability throughout the brain, especially when lower frequency (50 Hz) DBS was used. However, after DBS, all neurophysiological markers remained significantly lower than in healthy controls and objective increases in consciousness remained limited.
Inspiring future research
In conclusion, this study shows that DBS can re-activate dormant functional brain networks, even years after injury, but that the severely injured brain still lacks the ability to serve cognitive demands. This evidence inspires future research on DBS in patients with PDOC, especially in those patients who have more intact brain networks. A larger sample of patients is necessary to build further on these preliminary findings.
Source: Scientific Reports