Five years ago, a similar seminar was published by Scheltens. Comparing the two papers illustrates the progress that has been made since then. Research on the underlying pathology, the recognition of multiple causative and protective genes, the identification of new blood-based and imaging biomarkers have brought many new insights. And even the first cautious signals of positive effects of disease modifying treatments and lifestyle interventions are reported.
Prevalence and impact
Alzheimer’s disease is the leading cause of dementia. Most recent data indicate that, by 2050, the prevalence of dementia will double in Europe and triple worldwide. This estimate is three times higher when the diagnosis is based on a biological, rather than a clinical definition of Alzheimer's disease. Which makes Alzheimer’s one of the most expensive, lethal, and burdening diseases of this century.
Disease etiology
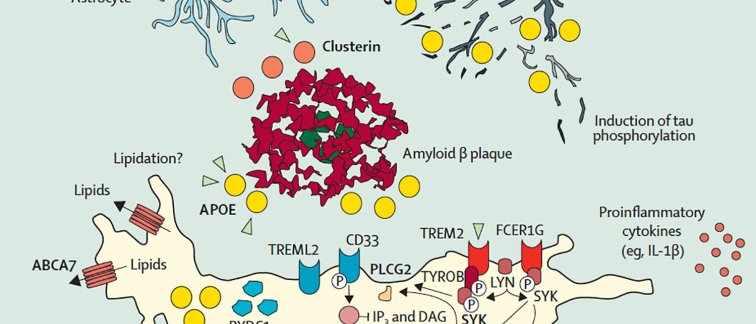
Research of the past five years has contributed to a better understanding of the underlying pathology of the disease. The earliest phase of Alzheimer's disease (cellular phase) happens in parallel with accumulating amyloid β, inducing the spread of tau pathology. The risk of Alzheimer's disease is 60–80% dependent on heritable factors, with more than 40 Alzheimer's disease-associated genetic risk loci already identified, of which the APOE alleles have the strongest association with the disease.
Diagnostics and prevention
Novel biomarkers include PET scans and plasma assays for amyloid β and phosphorylated tau, which show great promise for clinical and research use. Multidomain lifestyle-based prevention trials suggest cognitive benefits in participants with increased risk of dementia. Lifestyle factors do not directly affect Alzheimer's disease pathology, but can still contribute to a positive outcome in individuals with Alzheimer's disease. Promising pharmacological treatments are poised at advanced stages of clinical trials and include anti-amyloid β, anti-tau, and anti-inflammatory strategies.
Read the article in The Lancet.